
Nội dung bài viết / Table of Contents
This post is also available in:
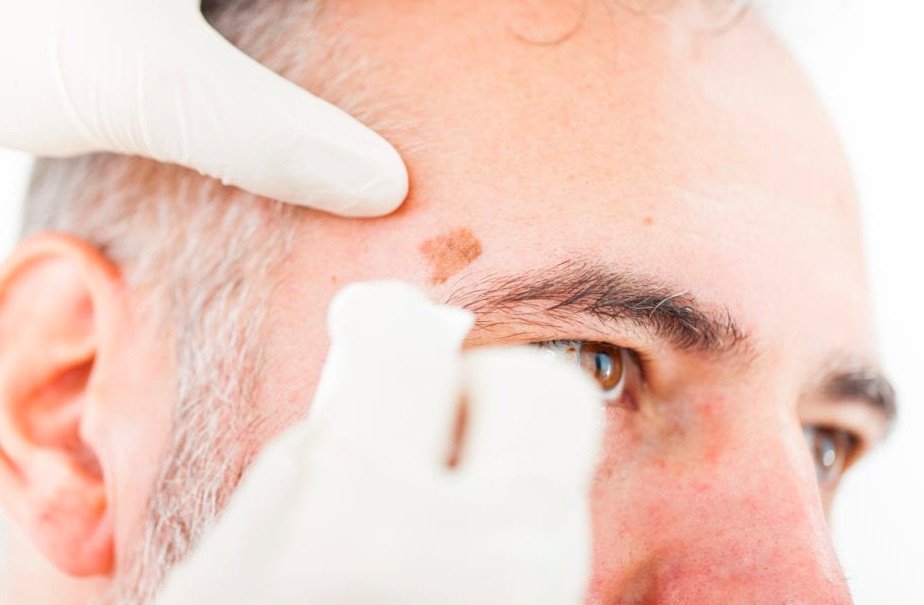
Actinic keratosis, also called solar keratosis, is a rough, scaly patch on your skin that develops in sun-exposed skin, especially on the face, hands, forearms, and the neck. It is seen most often in pale-skinned, fair-haired, light-eyed people.
In most cases, actinic keratosis is not cancerous. They are considered “in situ” stage squamous cell carcinoma lesions which mean the lesions are confined to one location and not invading other tissues.
The closer to the equator you live, the more likely you are to have actinic keratosis. The incidence is slightly higher in men, because they tend to spend more time in the sun and use less sun protection than women do.
However, it can be managed by reducing your risk factors. Please discuss with your doctor for further information.
Actinic keratosis starts out as thick, scaly, crusty skin patches which are usually about the size of a small pencil eraser. There might be itching or burning in the affected area.
Over time, the lesions can disappear, enlarge, remain the same, or develop into squamous cell carcinoma. There is no way of knowing which lesions may become cancerous.
The signs and symptoms of an actinic keratosis include:
It can be quite difficult to distinguish between noncancerous spots and cancerous ones. So it is considered that you should have your skin evaluated by a doctor — especially if a spot or lesion persists, grows or bleeds.
If you have any signs or symptoms listed above or have any questions, please consulting with your doctor. Everyone’s body acts differently. It is always best to discuss with your doctor what is best for your situation.
There are a great number of causes of this condition; however, long-term exposure to sunlight is considered as one of the most common causes to induce actinic keratosis, which is also called solar keratosis, is a skin growth that develops in sun-exposed skin, especially on the face, hands, forearms, and the neck.
It is seen most often in pale-skinned, fair-haired, light-eyed people, beginning at age 30 or 40 and becoming more common with age.
The ultraviolet radiation given off by the lamps in a tanning salon can be even more dangerous than the sun, so dermatologists warn against indoor tanning.
Occasionally, actinic keratosis may be caused by extensive exposure to X-rays or a number of industrial chemicals.
You may have a higher risk of developing this condition if you:
The information provided is not a substitute for any medical advice. ALWAYS consult with your doctor for more information.
Your doctor will likely be able to determine whether you have an actinic keratosis simply by examining your skin with using a bright light or magnifying lens to look for growths, moles, or lesions.
If there is any doubt, they may do other tests, such as a skin biopsy. During a skin biopsy, your doctor takes a small sample of your skin for analysis in a lab.
Even after treatment for actinic keratosis, your doctor will likely suggest that you have your skin checked at least once a year for signs of skin cancer.
Almost all actinic keratosis can be eliminated if treated early before they become skin cancers. Various treatment options are available, which depend on the growth’s characteristics and the patient’s age and health.
Some of these strategies increase sun sensitivity, so check with your doctor, and be especially diligent about using sun protection during the treatment period. Common treatments include the following.
Read more posst:
What are some lifestyle changes or home remedies that can help me manage actinic keratosis?
The best way to prevent actinic keratosis is to protect yourself from the sun. Here are some sun-safety habits that really work:
If you have any questions, please consult with your doctor to better understand the best solution for you.
Sources: